Many expectant mothers face conflicting advice about eating during labor, leaving them uncertain about what’s safe and beneficial. Hospital policies vary widely, and outdated guidelines often clash with modern evidence-based practices. Understanding your nutrition and hydration options during labor empowers you to make informed decisions that support your energy, comfort, and birth experience. This guide provides clear, research-backed recommendations on what you can safely consume throughout different labor stages, helping you and your partner prepare for a more confident childbirth journey.
Table of Contents
- Key takeaways
- Understanding the history and current guidelines about eating during labor
- What you can eat and drink safely during labor
- How eating during labor affects you and your baby
- Tips for managing nutrition and hydration during different labor stages
- Explore doula support for a more empowered labor experience
- Frequently asked questions about eating during labor
Key Takeaways
| Point | Details |
|---|---|
| Policy variation across settings | Hospital policies vary widely, so verify current guidelines with your care team and doulas before and during labor. |
| Light foods advised | Light easily digestible foods are generally advised in early and active labor to maintain energy without overloading the system. |
| Stay hydrated during labor | Hydration is important throughout labor with water as the primary option and electrolyte drinks as a consideration for longer labors. |
| Consult care team | Consult with healthcare providers and doulas to tailor nutrition plans to your risk level pain management and birth setting. |
Understanding the history and current guidelines about eating during labor
For decades, laboring women faced strict fasting requirements based on concerns about anesthesia complications. Historically, women in labor were advised strict fasting to reduce aspiration risk during anesthesia, a practice rooted in outdated surgical protocols from the mid-20th century. These blanket restrictions ignored the physical demands of labor, which can last many hours and require significant energy reserves.
Modern obstetric care has shifted dramatically. Research now recognizes that labor is an athletic event requiring fuel and hydration to sustain contractions and maintain maternal wellbeing. Current medical guidelines acknowledge that complete fasting may do more harm than good for low-risk births, potentially leading to dehydration, ketosis, and exhaustion that can complicate labor progress.
However, policies remain inconsistent across birth settings. Some hospitals maintain conservative restrictions, especially when epidural anesthesia or cesarean delivery becomes likely. Birth centers and home birth settings typically offer more flexibility, trusting women to listen to their bodies. Understanding these variations helps you advocate for preferences while respecting legitimate safety concerns.
Key factors influencing current eating guidelines include:
- Risk level of your pregnancy and anticipated delivery method
- Type of pain management planned, particularly epidural or general anesthesia
- Hospital protocols and anesthesiologist preferences
- Labor progression speed and any complications that arise
- Your personal comfort level and hunger cues throughout labor
Working with doula support during labor can help you navigate these policies while ensuring your needs are heard. Doulas understand how to balance institutional requirements with your desire for autonomy and comfort. They can also help communicate your preferences to medical staff and suggest alternatives when restrictions apply. Reviewing a comprehensive nutrition guide during labor before your due date ensures you’re prepared with evidence-based information to discuss with your care team.
What you can eat and drink safely during labor
Choosing appropriate foods and beverages during labor requires balancing nourishment with digestive comfort. Light, easily digestible foods and clear fluids are generally advised in early and active labor stages, providing energy without overwhelming your system during intense physical work.

Clear liquids form the foundation of labor nutrition. Water remains your best option, keeping you hydrated without adding sugar or artificial ingredients. Electrolyte drinks help replace minerals lost through sweating and exertion, particularly during longer labors. Herbal teas like chamomile or peppermint can soothe nerves and settle your stomach. Coconut water offers natural electrolytes with a mild flavor that many women tolerate well.
When it comes to solid foods, simplicity wins. Fresh fruit provides quick energy through natural sugars plus vitamins and fiber. Berries, melon, and grapes are especially refreshing and easy to eat between contractions. Whole grain crackers or toast offer sustained energy from complex carbohydrates without feeling heavy. Honey can provide an instant glucose boost if you need quick fuel. Popsicles serve double duty, offering hydration and a cooling sensation that many laboring women find comforting.
Foods to avoid during labor:
- Heavy, greasy items like burgers or fried foods that slow digestion
- Dairy products that may increase nausea or mucus production
- Spicy dishes that could cause heartburn or stomach upset
- Very sugary snacks that lead to energy crashes
- Large portions that make you feel uncomfortably full
Pro Tip: Pack a labor bag with approved snacks like applesauce pouches, energy balls made with dates and nuts, or honey sticks for quick energy hits. Having options ready prevents last-minute scrambling and ensures you have foods you actually want to eat.
Your care team’s recommendations should guide final decisions. Some hospitals restrict all solid food once active labor begins or if you request an epidural. Others allow light eating throughout uncomplicated labor. Preparing your body for labor nutrition includes discussing these policies at prenatal appointments so you understand what to expect. If restrictions feel unnecessarily limiting, ask about the specific reasoning and whether alternatives exist. Reviewing labor nutrition recommendations helps you arrive informed and ready to advocate for reasonable accommodations.
How eating during labor affects you and your baby
The physiological impact of nutrition during labor extends beyond simple hunger satisfaction. Proper hydration and light nutrition help maintain maternal strength and focus, which can improve labor effectiveness by providing the glucose and fluids your muscles need for sustained contractions.
Your body burns tremendous calories during labor, comparable to running a marathon. Without adequate fuel, you risk developing ketosis, a metabolic state where your body breaks down fat for energy, producing ketones that can make you feel weak, nauseous, and mentally foggy. This metabolic shift may slow labor progress and reduce your ability to cope with contractions effectively.
Dehydration compounds these challenges. Even mild fluid deficits can trigger headaches, dizziness, and reduced blood volume that affects placental blood flow. Your baby depends on consistent oxygen and nutrient delivery through the placenta, making maternal hydration critical for fetal wellbeing. Adequate fluids also help maintain amniotic fluid levels and support your body’s natural oxytocin production.
How nutrition impacts your labor experience:
- Energy levels directly influence your ability to work with contractions rather than fight them
- Blood sugar stability affects mood, reducing anxiety and irritability during intense moments
- Hydration status determines how well your body responds to natural labor hormones
- Digestive comfort influences your ability to move freely and find comfortable positions
- Nutritional choices either support or hinder your mental focus and emotional resilience
The aspiration concern that drives fasting policies deserves context. In uncomplicated vaginal births with regional anesthesia like epidurals, aspiration risk remains extremely low. General anesthesia, rarely needed except for emergency cesareans, carries higher risk because it eliminates protective airway reflexes. Modern anesthetic techniques and rapid sequence induction have made aspiration complications increasingly rare, even when women have eaten lightly.
“Labor is physical work that requires fuel. Denying nutrition based on unlikely complications can create more problems than it prevents for most healthy pregnancies.”
Some foods genuinely increase discomfort during labor. Greasy or high-fat items sit heavily in your stomach, potentially causing nausea as labor intensifies. Very acidic foods may trigger heartburn, especially as your baby presses upward against your diaphragm. Listening to your body’s signals helps you choose foods that energize rather than upset you. Creating calm birth space includes having the right nutrition options available so you can focus on labor rather than hunger or thirst. Understanding the nutrition impact on labor empowers you to make choices that support both your immediate comfort and your body’s long-term needs through delivery and recovery.
Tips for managing nutrition and hydration during different labor stages
Labor progresses through distinct phases, each with different nutritional needs and practical considerations. Nutrition needs and hospital policies often change throughout labor’s progression, requiring adaptable strategies that respond to your body’s changing demands.
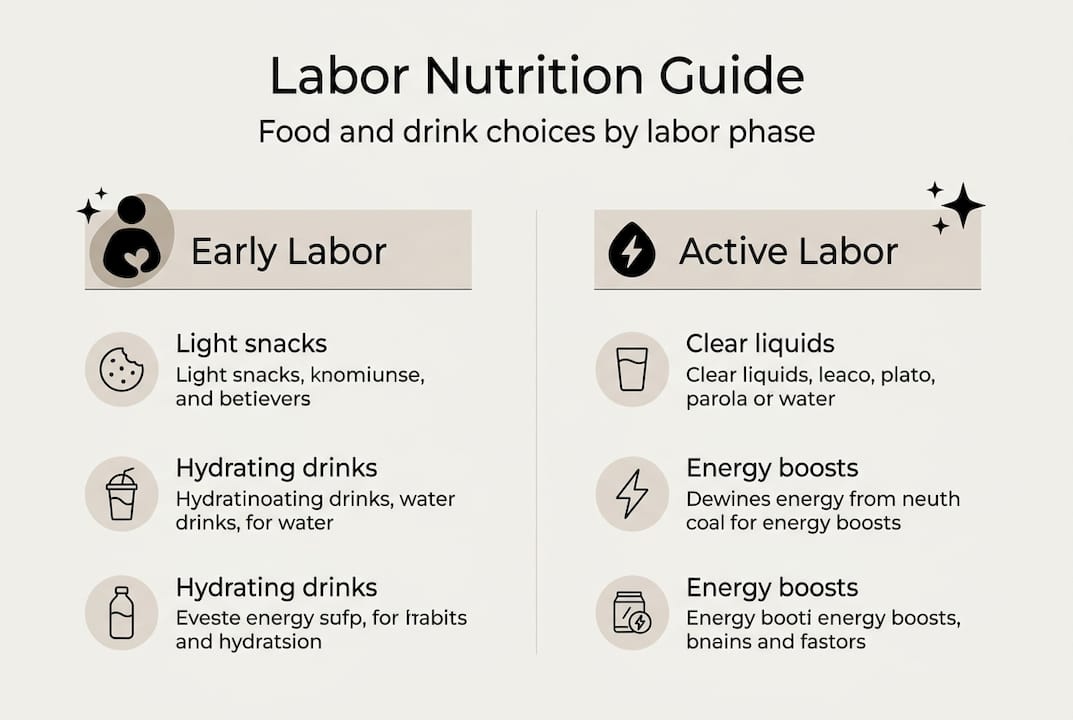

Early labor typically spans hours or even days for first-time mothers. During this phase, eating regular light meals maintains your energy reserves for the work ahead. Focus on foods you genuinely enjoy and that sit well in your stomach. This is not the time to experiment with new flavors or cuisines. Stick with familiar, comforting options that you know your body tolerates.
As contractions intensify into active labor, your appetite naturally decreases. Most women lose interest in solid food as their body redirects energy toward the birth process. Hydration becomes paramount during this phase. Sipping fluids between contractions prevents dehydration without making you uncomfortably full. Small bites of easily digestible foods like fruit or crackers provide quick energy if you feel hungry.
Transitional labor, the most intense phase before pushing, usually involves minimal eating. Nausea often accompanies this stage as your cervix completes dilation. Ice chips, small sips of water, or sucking on popsicles may be all you can manage. This is normal and expected. Your body has shifted entirely into birth mode.
| Labor Stage | Recommended Nutrition | Hydration Focus | Practical Tips |
|---|---|---|---|
| Early labor | Light meals, whole grains, lean protein, fruit | Regular water intake, herbal tea | Eat normally, avoid heavy or spicy foods |
| Active labor | Small snacks, crackers, fruit, honey | Frequent small sips, electrolyte drinks | Follow hunger cues, prioritize hydration |
| Transition | Ice chips, popsicles if desired | Ice chips, small water sips | Focus on breathing, minimal intake |
| Pushing stage | Usually nothing | Ice chips only | All energy on delivery |
Practical preparation strategies:
- Pack a cooler with approved snacks and drinks for your birth location
- Label items clearly so support people know what’s available
- Include straws or sports bottles for easy drinking during contractions
- Bring multiple flavor options since preferences may shift during labor
- Discuss your nutrition plan with your care team before labor begins
Pro Tip: Freeze small portions of coconut water or diluted juice in ice cube trays. These provide hydration and electrolytes while offering a cooling sensation that many laboring women find soothing. Partners can offer them easily without requiring you to drink from a cup.
Your support team plays a crucial role in nutrition management. Partners can track your fluid intake, offer snacks at appropriate times, and advocate for your preferences with medical staff. Postpartum and labor nutrition care extends beyond delivery, but establishing good habits during labor sets the foundation for recovery. A doula can remind you to drink regularly, suggest position changes that ease digestion, and help you communicate with nurses about your needs. They understand the balance between following hospital protocols and ensuring you receive adequate nourishment throughout your birth experience.
Explore doula support for a more empowered labor experience
Navigating nutrition decisions during labor becomes easier with experienced support by your side. Professional doulas provide continuous encouragement and evidence-based guidance throughout your birth journey, including personalized advice on eating and drinking that aligns with your specific circumstances and preferences.
Serenity Doula offers pregnancy and birth support tailored to your unique needs, helping you prepare physically and emotionally for labor while understanding what a doula does to support your choices. Our childbirth education services provide comprehensive preparation covering nutrition strategies, comfort measures, and communication techniques that empower you to advocate for your preferences. Whether you’re planning a hospital birth, birth center delivery, or home birth, having a knowledgeable doula helps you make informed decisions about eating during labor while ensuring your voice is heard throughout the process.
Frequently asked questions about eating during labor
Is it safe to eat during early labor?
Yes, eating light, easily digestible foods during early labor is generally safe and beneficial for most women. Focus on foods that provide sustained energy without causing digestive discomfort, and stay well hydrated with water or clear fluids.
What happens if I eat too much during labor?
Eating large or heavy meals during labor can cause nausea, vomiting, or uncomfortable fullness that makes coping with contractions more difficult. Stick to small portions of simple foods and listen to your body’s signals about what feels right.
Can I drink coffee or juice during labor?
Clear apple juice or diluted fruit juice is usually acceptable, providing quick energy from natural sugars. Coffee may be restricted at some hospitals due to caffeine content and acidity, so check your facility’s specific policies beforehand.
Why do some hospitals not allow eating during labor?
Hospital restrictions stem from concerns about aspiration risk if emergency general anesthesia becomes necessary. While this risk is extremely low in uncomplicated births, institutional policies often take a conservative approach to minimize any potential complications.
How can a doula help with nutrition during labor?
A doula can remind you to stay hydrated, offer appropriate snacks at the right times, and advocate for your nutrition preferences with medical staff. They understand hospital policies while prioritizing your comfort and energy needs throughout labor support.
What should I eat right before going to the hospital?
Eat a light, balanced meal with complex carbohydrates and lean protein before heading to the hospital, similar to what you’d consume before athletic activity. Avoid heavy, greasy, or very spicy foods that might cause digestive issues during labor.