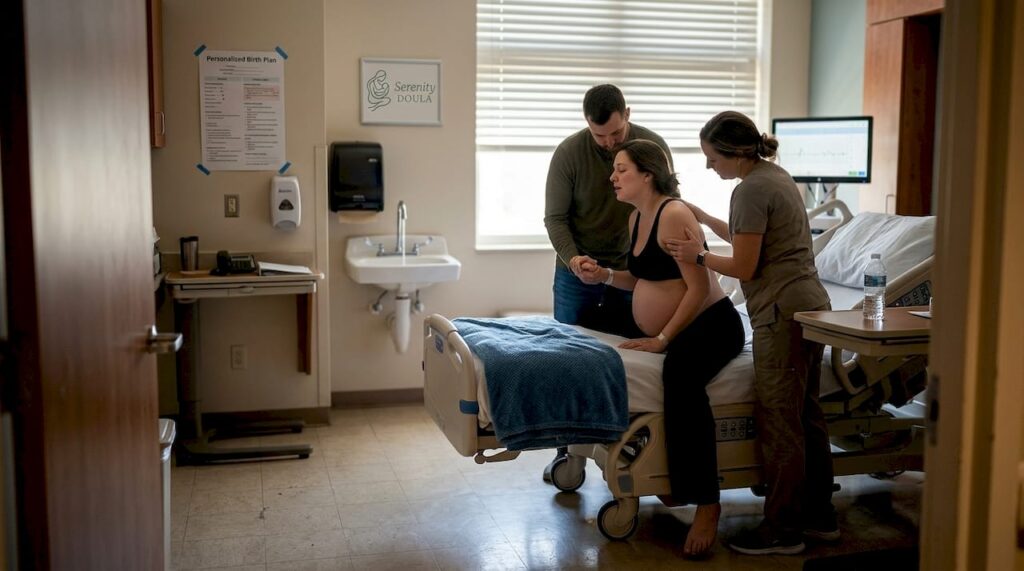
Many expectant parents assume hospital birth is their only safe choice, but Bucks and Montgomery counties offer diverse birthing environments with midwife and doula support. Hospital birthing rooms, birth centers, and home births each provide unique benefits for holistic, personalized care. Recent changes like Grand View’s temporary closure and Lifecycle’s planned 2026 closing require careful planning. This guide clarifies your options to help you create a confident, informed birthing experience tailored to your family’s needs.
Table of Contents
- Exploring Birthing Room Options In Bucks And Montgomery Counties
- Understanding The Role Of Doulas And Midwives In Your Birthing Room
- Comparing Holistic Birthing Environments: Home, Birth Center, And Hospital
- Planning Your Personalized Birthing Experience With Doula Support
- How Serenity Doula Supports Your Birthing Journey
- Frequently Asked Questions About Birthing Rooms And Doula Support
Key takeaways
| Point | Details |
|---|---|
| Hospital birthing rooms | Private spaces with medical backup, midwife support, and low intervention rates at Einstein Montgomery. |
| Home and birth center births | Holistic, lower-intervention experiences with continuous doula and midwife care for personalized support. |
| Doula support benefits | Emotional, physical, and educational assistance reduces interventions and improves satisfaction during labor. |
| Local facility changes | Grand View’s temporary closure and Lifecycle’s 2026 closing require early planning for alternative birthing locations. |
| Postpartum resources | Local doula postpartum care and mental health support address recovery needs and screening for depression. |
Exploring birthing room options in Bucks and Montgomery counties
Birthing rooms in Bucks and Montgomery counties range from hospital settings with medical backup to intimate home environments with holistic care. Hospital birthing rooms provide private labor, delivery, and recovery spaces with access to emergency interventions and neonatal intensive care when needed. Einstein Montgomery shows 65% midwife-attended births with low cesarean rates and strong breastfeeding support, demonstrating how hospitals can integrate holistic practices. These rooms typically include monitoring equipment, pain relief options, and immediate access to obstetricians if complications arise.
Recent changes affect local availability. Grand View’s labor unit closed temporarily in late 2025, redirecting births to other facilities. This closure highlights the importance of researching backup options early in pregnancy. Birth centers and home births coexist as alternatives, offering lower-intervention care with continuous doula support benefits throughout labor.
| Environment | Key features | Best for |
|---|---|---|
| Hospital | Medical backup, NICU access, midwife options | High-risk pregnancies, first-time parents wanting medical safety |
| Birth center | Water births, holistic care, lactation support | Low-risk pregnancies seeking less intervention |
| Home birth | Intimate setting, continuous midwife care, personalized environment | Healthy pregnancies desiring maximum autonomy |
Choosing your birthing room involves weighing several factors:
- Medical history and risk level determine safety requirements
- Desired intervention level affects environment choice
- Distance to emergency care matters for home and birth center births
- Insurance coverage varies by birthing location
- Personal comfort with different settings influences satisfaction
Each environment supports different philosophies of birth. Hospitals prioritize safety with intervention readiness, birth centers balance holistic care with medical protocols, and home births emphasize physiological birth in familiar surroundings. Your choice should align with your health profile, values, and comfort level with medical technology.
Understanding the role of doulas and midwives in your birthing room
Doulas and midwives transform the birthing experience through continuous, personalized support across all environments. Doulas provide physical, emotional, and educational support including comfort techniques, encouragement, and birth education throughout labor. Unlike medical staff who rotate shifts, doulas remain with you from early labor through delivery, creating consistency and trust. Their presence complements rather than replaces medical care, filling gaps in emotional support that busy hospital staff cannot always provide.

Comfort techniques doulas use include positioning suggestions, counter-pressure for back labor, rebozo sifting to help baby position, and breathing guidance. They encourage movement using labor balls, walking, and position changes that work with gravity to progress labor naturally. Midwives similarly promote physiological birth through hands-on care, supporting vaginal birth after cesarean attempts, and minimizing unnecessary interventions. Both professionals recognize birth as a normal process requiring support rather than routine medical management.
Research demonstrates measurable benefits. Doula support links to shorter labors, fewer cesarean sections, lower epidural rates, and higher satisfaction scores. Parents report feeling more confident, informed, and empowered when continuous support is present. The emotional reassurance doulas provide reduces anxiety, which can slow labor progress and increase intervention needs.
Doulas support you through:
- Physical comfort with massage, positioning, and pain management techniques
- Emotional reassurance during challenging labor moments and decision-making
- Educational guidance explaining procedures and helping you understand options
Pro Tip: Share your birth plan with your doula weeks before delivery to ensure they understand your priorities and can advocate effectively during labor when communication becomes difficult.
The partnership between doulas and medical staff creates optimal outcomes. Doulas focus on your emotional and physical comfort while midwives and doctors manage clinical care. This team approach ensures you receive both compassionate support and medical expertise. In hospital settings, doulas help you navigate institutional protocols while maintaining your preferences. At home or birth centers, they provide additional hands for comfort measures while midwives monitor clinical progress.
Communicating clearly with your entire care team maximizes support effectiveness. Introduce your doula to medical staff early, explain your preferences respectfully, and remain flexible as labor unfolds. The best outcomes occur when everyone works collaboratively toward your safe, satisfying birth experience.
Comparing holistic birthing environments: home, birth center, and hospital
Holistic birthing environments prioritize physiological birth, minimal intervention, and family-centered care across different settings. Hospital births at facilities like Einstein Montgomery offer medical safety with NICU backup while accommodating midwife care and doula support. Private labor and delivery rooms allow family presence, and hospitals increasingly support natural birth preferences including delayed cord clamping, immediate skin-to-skin contact, and movement during labor. Medical backup remains immediately available if complications arise, providing security for parents concerned about emergency scenarios.
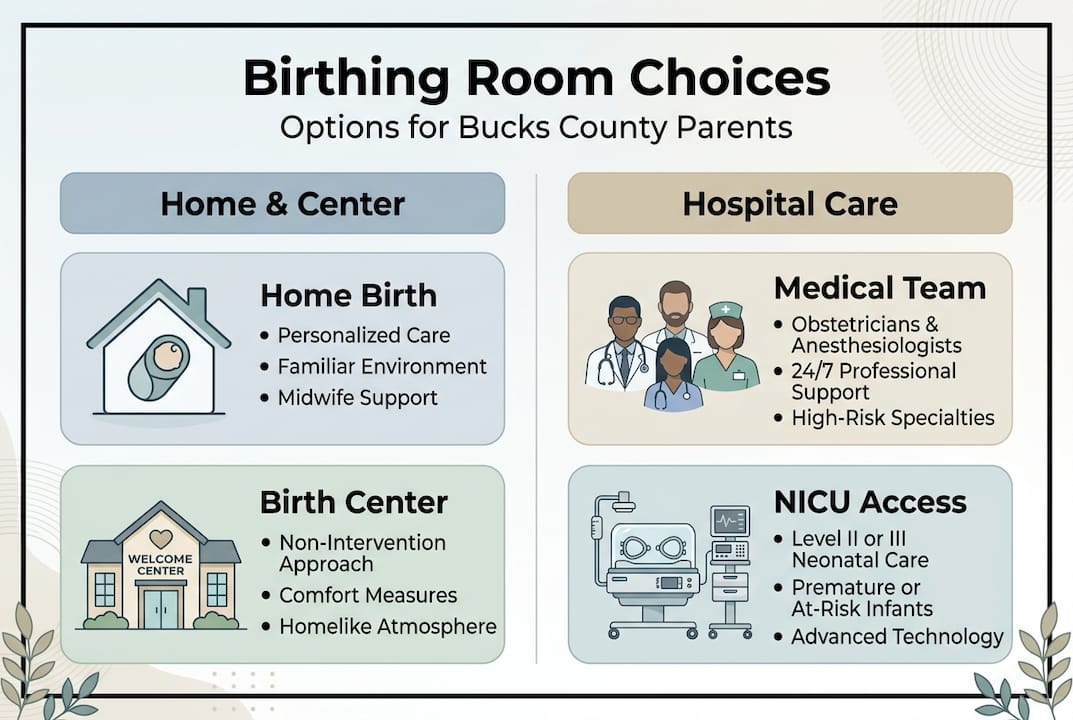
Birth centers deliver holistic, lower-intervention care in homelike settings. Lifecycle birth center offers water births and lactation support, having delivered over 16,000 babies before its planned 2026 closing. These facilities provide comfortable environments with midwife-led care, encouraging physiological birth without routine interventions. Birth centers suit healthy, low-risk pregnancies where parents desire less medical management but want nearby hospital transfer capability. However, they lack immediate access to operating rooms or advanced neonatal care, requiring transfer for emergencies.
Home births provide intimate, personalized care in your own space. Home birth midwives offer 24/7 availability with 6-8 weeks postpartum support and continuous doula-like care throughout labor. You control your environment completely, choosing lighting, music, food, and who attends. Midwives bring necessary equipment including oxygen, resuscitation tools, and monitoring devices. Home birth suits very low-risk pregnancies with parents committed to physiological birth and comfortable with distance from hospital resources.
| Environment | Intervention rate | Support type | Postpartum care |
|---|---|---|---|
| Hospital | Moderate to high | Midwife, doula, OB available | 24-48 hour stay, lactation consults |
| Birth center | Very low | Midwife, doula | 6-12 hour stay, follow-up home visits |
| Home birth | Minimal | Midwife, doula | Immediate postpartum home visits, extended support |
Choosing your birthing environment requires these steps:
- Assess your medical history and risk factors with your healthcare provider
- Tour available facilities or interview home birth midwives to understand care philosophies
- Verify insurance coverage for your preferred setting and backup plans
- Consider travel time to hospitals from birth centers or home for emergency transfers
- Match your birth preferences with the environment’s typical practices and flexibility
Pro Tip: Plan early due to Lifecycle’s 2026 closing and Grand View’s temporary closure to secure your preferred birthing location and avoid last-minute scrambling for alternatives.
Postpartum support varies significantly by environment. Hospitals provide immediate lactation help and newborn screening but shorter stays limit bonding time. Birth centers offer initial postpartum checks before discharge and home visits within days. Home births include extended postpartum midwife visits addressing recovery, breastfeeding, and newborn care. Adding postpartum doula support enhances recovery across all settings by providing practical help, emotional support, and monitoring for complications.
Your choice ultimately reflects your values, risk tolerance, and vision for birth. Each environment can support holistic care when you communicate preferences clearly and build a supportive team. Consider visiting calm birth space tips to personalize any setting for comfort and peace.
Planning your personalized birthing experience with doula support
Creating your ideal birthing experience requires early preparation, clear communication, and professional support throughout pregnancy and postpartum. Start by touring facilities or scheduling consultations with doulas and midwives during your second trimester. First-time parents especially benefit from doula education, birth plan preparation, and postpartum guidance. These early conversations help you understand care philosophies, ask questions without pressure, and build relationships before labor begins.
Develop a flexible birth plan documenting your preferences for interventions, pain management, support people, and immediate postpartum care. Include your priorities for movement during labor, monitoring methods, and newborn procedures like delayed cord clamping or immediate breastfeeding. Share this plan with your doula, midwife, and hospital staff well before your due date. A good birth plan communicates preferences while acknowledging that labor may require adjustments.
Leverage doula services for continuous support from pregnancy through postpartum. Prenatal visits with your doula cover comfort techniques, birth education, and planning conversations. During labor, doulas provide physical comfort measures, emotional reassurance, and help communicating with medical staff. Their presence creates calm, reduces anxiety, and helps you stay focused on your body’s signals.
Postpartum doula care addresses recovery, newborn care, and mental health needs often overlooked after birth. Doulas assist with breastfeeding challenges, infant soothing, light household tasks, and sibling adjustment. They screen for postpartum depression and anxiety, connecting families with resources when needed. Montgomery County offers free support via 1-888-404-0620 for postpartum depression screening and counseling.
Essential preparation steps include:
- Research local birthing facilities and interview potential doulas by your second trimester
- Attend childbirth education classes to understand labor stages and comfort techniques
- Draft a birth plan reflecting your priorities while remaining flexible for medical needs
- Arrange postpartum support including doula care, lactation consultants, and mental health resources
- Create backup plans for facility closures or unexpected transfers during labor
Pro Tip: Communicate openly with all caregivers throughout pregnancy and update your birth plan as circumstances or preferences evolve to ensure everyone supports your current needs.
Integrating professional support with your birthing environment choice maximizes satisfaction and outcomes. Doulas work effectively in hospitals, birth centers, and homes, adapting their support to each setting’s protocols. They help you navigate institutional environments while maintaining your preferences and provide additional hands in less medicalized settings. This flexibility makes doula support valuable regardless of where you birth.
Postpartum planning deserves equal attention to birth planning. Arrange postpartum doula care before delivery, stock your home with recovery supplies, and identify mental health resources you can access quickly if needed. The fourth trimester challenges many families, and proactive support prevents crisis situations. Doulas provide practical help and emotional validation during this vulnerable transition, normalizing common struggles while identifying concerning symptoms requiring medical attention.
How Serenity Doula supports your birthing journey
Navigating birthing room choices and planning holistic care becomes simpler with experienced doula support. Serenity Doula offers comprehensive pregnancy to postpartum services tailored to your unique needs in Bucks and Montgomery counties. Our pregnancy and birth support includes prenatal education, continuous labor assistance, and immediate postpartum care across all birthing environments. We work seamlessly with hospital staff, birth center midwives, and home birth teams to enhance your experience.
Our childbirth education services prepare you with practical knowledge about labor stages, comfort techniques, and decision-making tools. We help you develop a birth plan reflecting your values while understanding when flexibility serves your safety. Postpartum support through our dedicated postpartum care addresses recovery, infant care, and mental health with compassionate, evidence-based guidance. Scheduling a consultation early ensures you have trusted support through every stage of your birthing journey.
Frequently asked questions about birthing rooms and doula support
What defines a birthing room and what should I expect?
A birthing room is a dedicated space for labor, delivery, and often recovery, designed to balance comfort with medical safety. Hospital birthing rooms include monitoring equipment and immediate intervention access, while birth center rooms emphasize homelike comfort with midwife-led care.
How do doulas complement midwives and medical staff?
Doulas provide continuous emotional and physical support while midwives and doctors manage clinical care. This partnership ensures you receive both compassionate comfort measures and medical expertise, with doulas filling support gaps that busy medical staff cannot always provide.
What should first-time parents know about choosing a birthing environment?
First-time parents benefit from touring multiple facilities, understanding intervention rates, and considering proximity to emergency care. Assess your risk level with your provider, verify insurance coverage, and choose an environment matching your comfort level with medical technology and intervention.
Are doulas available for postpartum support and mental health assistance?
Yes, postpartum doulas provide recovery support, newborn care guidance, and mental health screening during home visits. They help with breastfeeding challenges, monitor for postpartum depression signs, and connect families with professional resources when additional care is needed.
How do I prepare for changes like hospital or birth center closures?
Plan early by identifying backup facilities, discussing transfer protocols with your care team, and maintaining flexibility in your birth plan. Grand View’s temporary closure and Lifecycle’s 2026 closing require proactive research of alternative options to avoid last-minute stress during late pregnancy.